Clubfoot researchers have begun to report long-term data that continue to solidify the superiority of the conservative method over surgical intervention in most cases. But variations to the traditional Ponseti method are arising, particularly in developing countries, and may alter outcomes.
By Larry Hand
As most clinicians treating children for clubfoot have shifted over to the Ponseti method from comprehensive surgery, more information is surfacing on long-term outcomes, as well as short-term outcomes in lower- and middle-income countries.
Although many physicians say that, even today, practitioners should faithfully follow the method developed by the late orthopedist Ignacio Ponseti, MD, at the University of Iowa Hospitals and Clinics in Iowa City, some variations exist in daily practice and other variations are cropping up in published research papers. No one is arguing, however, about the effectiveness of the Ponseti method.
The traditional Ponseti method is ideally applied one to two weeks after birth and involves gently stretching the tendons and plaster casting the leg, changing the casts every four to seven days for about eight weeks. Often, prior to the last cast, a physician will perform a tenotomy, snipping the heel cord; the child wears the final cast for two to three weeks. To prevent recurrence of the deformity, children then wear a brace consisting of shoes mounted on a bar for 23 hours a day for three months, and then at night for several years, usually until children are aged 3 to 5 years.
“The Ponseti method will always be best, as it spares the joints,” Angela M. Evans, PhD, senior lecturer in the Department of Podiatry at La Trobe University in Bundoora, Victoria, Australia, told LER in an email. “However, in more complicated cases [eg, arthrogryposis multiplex congenital] or very rigid cases, some surgery—mainly posterior release and Achilles lengthening—may be required. But initial casting may reduce the extent of surgery needed, which will likely be better in the longer term.”
“Surgery is almost a last resort, but nonetheless, every now and then it’s a necessary thing to do,” said Susan T. Mahan, MD, MPH, assistant professor of orthopedic surgery at Harvard Medical School in Boston.
Mahan, herself, uses the Ponseti method.
“I will attempt serial casting techniques in all patients with clubfoot, because I think the results of that are just the best,” she said. “The truth is that for most healthy kids, the Ponseti technique does terrifically. It’s really the rare kid that we end up having to reach for the surgical option.”
Long-term outcomes
Extensive surgical procedures involving soft tissue releases, which were popular before the advent of the Ponseti method, resulted in scarring, stiffness, and even overcorrection, which necessitated additional surgical procedures in many patients, according to David A. Spiegel, MD, associate professor of orthopedic surgery at the University of Pennsylvania Perelman School of Medicine in Philadelphia.
“In contrast,” he explained, “the Ponseti method is minimally invasive and does not disrupt joints and tends to preserve motion. Ponseti feet may be mildly undercorrected, but this is usually not apparent clinically. Basically what you’ve got is a foot that moves better and functions better over the long term into adulthood.”
Few studies have published long-term outcomes associated with the Ponseti method, but a case-controlled study reported in Clinical Orthopaedics and Related Research1 earlier this year (see LER:Pediatrics, February 2014, page 4) offers some details about long-term outcomes of the Ponseti method compared with comprehensive surgical release.
Researchers at the Shriner’s Hospital for Children in Chicago examined the records of individuals treated between 1983 and 1987 at two separate institutions with different treatment methods; 24 were surgically treated and 18 underwent the Ponseti method.
The Ponseti group had significantly greater ankle plantar flexion range of motion (ROM) and ankle plantar flexor and evertor strength, a lower incidence of ankle and foot osteoarthritis, and less pain compared with the surgical group. Both clubfoot groups had reduced ROM and more weakness and pain compared with controls who did not have clubfoot, findings that point to a need for better methods of improving these variables to achieve the best possible function in adulthood.
Undercorrection and overcorrection after Ponseti treatment can be hallmarks of congenital clubfoot, and problems can crop up in adulthood or at younger ages, according to a 2010 study.2 Issues included valgus deformities from overcorrection, varus deformities from undercorrection, and degenerative conditions such as arthritis that may result from the underlying congenital deformity or its treatment.
Global popularity
Now that the Ponseti method has reached global popularity, some variations in protocols and methods have evolved. In a systematic review published in April 2014 in Clinical Orthopaedics and Related Research,3 Chinese researchers delved into reported variations in manipulation, casting, and percutaneous Achilles tenotomy, as well as whether bracing type and protocol made a difference in relapse prevention.
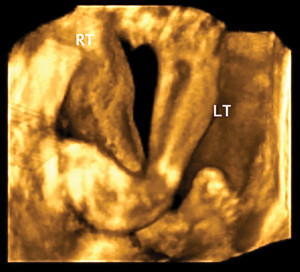
A prenatal ultrasound image of a child with bilateral clubfoot. (Image courtesy of the Boston Children’s Hospital Department of Orthopedics.)
Of the 19 studies evaluated, they found that researchers described their methods poorly in 11 and clinicians didn’t follow the main Ponseti principles in three. The brace deviated from the recommended type in three studies, and in another three, the prescribed brace wear times differed from those of the traditional Ponseti method. In addition, indications for recognition of relapse and its management differed from the traditional Ponseti method in some studies. The researchers concluded that clinically important variations in outcomes might have resulted from deviations from the traditional Ponseti method’s manipulation, casting, tenotomy, and bracing techniques and relapse recognition and management protocols.
In the same journal the following month,4 Spiegel called for journals to require that, “as a minimum,” authors provide detailed treatment protocols in their methods sections so that the results of different studies can be adequately compared.
“Do it exactly as the man says, or don’t say you’re doing the Ponseti method,” Spiegel said.
That has already begun to happen with some researchers—many of whom have had to adapt protocols to accommodate challenging conditions in developing areas around the globe.
“The impact of Ponseti casting on low-income countries is exciting,” said Luke S. Harmer, MD, MPH, an orthopedic trauma fellow at Carolinas Medical Center in Charlotte, NC. While at the University of Calgary in Alberta, Canada, he coauthored a paper on providing care in these areas.5
“With this [Ponseti] technique we are able to treat children with a low-tech, low-risk, low-infrastructure method that provides results better than our previous surgical algorithm,” he said.
Evans’ group in Australia has been conducting a sustainable clubfoot program in Bangladesh called Walk for Life (WFL).6 Since 2009, the group has been evaluating Ponseti clubfoot treatment in children using a Bangla clubfoot tool, a measuring system they
developed based on existing validated instruments and adapted to local factors, including overcrowded clinics, difficulty traveling to clinics, lack of basic facilities, and poor healthcare infrastructure. The Bangla tool incorporates three domains: parent satisfaction determined by interview, gait function, and clinical foot evaluation.
In an evaluation of the first 5000 feet treated in the program,7 Evans and colleagues found that the WFL results demonstrate that “rapid case ascertainment is possible in a developing world setting with appropriate logistical support.” Among the adaptations to local factors was the use of physiotherapists and paramedics to do the casting, along with ongoing training and regular clinical review of their technique by physicians.
In a two-year review of the WFL program, epublished in May 2014 by the Journal of Pediatric Orthopaedics,8 Evans and colleagues described results achieved at the 10 largest WFL clinics. Among 400 cases selected randomly from 1442 children, 99% could walk independently. According to Bangla clubfoot tool scores, parents were highly satisfied but said the cost of the treatment (3000 Taka, or $38.48) was not affordable.
“We found that if the treatment were not free, most children would not have had access, and so would not be corrected and walking,” Evans said. “We estimate there are some five thousand new cases born annually [in Bangladesh]. The significance of clubfoot is enormous in the developing world where walking avails working and earning, or not.”
Among local adaptations to traditional Ponseti methods, she said, are more frequent cast changes in which each cast stays on for about three days rather than a week.
“It can at least halve the time a baby is in plaster. We used this in [the Polynesian kingdom of] Tonga and wrote up the cases,”9 she said.
In that paper,9 Evans and colleagues reported two cases of “fast casting” in which children were cast and recast four times in one week followed by tenotomy, with both babies showing consistent correction of the foot deformity 10 weeks after start of treatment. The researchers noted they used “more rather than less” manipulation prior to casting.
Rosalind Owen, BSc, MSc, of the Institute of Child Health at University College London, UK, said, “One variation which has shown comparable results to Ponseti is the ‘accelerated Ponseti technique.’ This has shown good outcomes in Malawi and reduced the amount of time parents accompanying children for treatment have to stay away from their work and families.”
In that Malawi randomized clinical trial,10 researchers found no significant outcome differences among 40 patients (61 feet) who were randomized to either standard weekly cast changes or to changes three times a week. The median number of days in plaster was 16 for the accelerated group, compared with 42 for the control group, and researchers followed 36 of the 40 patients for six months. Researchers said it is too early to know how or if fast casts would affect long-term outcomes.
Context
In a 2012 review of clubfoot treatment outcomes in low- and middle-income countries,11 Owen and colleague Gayatri Kembhavi, PhD, found the Ponseti method was more effective than other conservative techniques but not directly comparable to surgery. They found that “contextual factors” influenced outcomes, but that clinicians who used the Ponseti method took more measures to overcome those factors than did clinicians using other techniques.
The factors include resources needed to provide care, materials needed for treatment, appropriate training for providers, and parents’ abilities to collaborate with providers.
Some variations can have negative effects, Owen said.
“Incorrect ‘Ponseti-style’ treatment can include using below-knee casts,12 not using the foot abduction brace [or not using it long enough], not doing tenotomy, and failure to identify the lateral head of talus and use it as the fulcrum of movement in casting,” she said. “These would result in probable slipping of the casts and noncorrection of the deformity, relapse of deformity, incomplete correction of deformity, and ineffective manipulation and casting, respectively. These are only some of the variations with negative outcomes.”
But not all variations have such consequences, Mahan of Harvard said.
“I think there will always be some variations in everyone’s interpretation [of the Ponseti technique],” she said. “One basic variation is whether to use plaster or fiberglass casts. The type of bracing and the length of bracing that’s done after serial casting is another variation. Some kids will get a tenotomy and some kids won’t. I think most of us follow Ponseti guidelines, but even within his guidelines, there’s some wiggle room for variation.”
Ponseti vs open surgery
In a meta-analysis published in 2013 in the World Journal of Orthopedics,13 researchers analyzed results from 12 studies published between January 1950 and October 2011 comparing clubfoot treatment with the Ponseti method or open surgery. They found that, while patients managed with the Ponseti method had higher rates of excellent or good outcomes than surgical patients, the difference barely missed statistical significance (p = .053). Still, they recommend the Ponseti method. Follow-up in the studies averaged 15.7 years.
“Serial manipulation and casting has been widely accepted as the initial treatment of idiopathic clubfeet, and surgical soft-tissue release is reserved for clubfeet that cannot be completely corrected, in case of relapse of the deformity or in case of nonidiopathic clubfoot, such as clubfoot associated with arthrogryposis,” lead author Marios G. Lykissas, MD, PhD, a pediatric orthopedic surgeon at Cincinnati Children’s Hospital Medical Center in Cincinnati, OH, told LER in an email.
The researchers found a correlation between a larger anteroposterior talocalcaneal angle and higher rates of excellent or good results, but no other significant correlations with functional or radiographic outcomes.
“Noncompliance of the family to follow the brace protocol is associated with unexpected high recurrence rate ranging from thirty to forty five percent and subsequent early onset arthrosis and pain if the recurrence is left untreated,” Lykissas explained. “There is no association between poor bracing compliance and families’ educational level, income, or cultural origin. Distance from the treatment centers and accessibility to the healthcare system are important parameters that may also adversely affect compliance, and secondarily, the success rate. In addition, concurrent illnesses may affect management of clubfeet with the Ponseti method.”
As always, compliance
“Compliance with casting and, even more importantly, boots-and-bars bracing, is important to outcomes,” Luke Harmer said. “This is part of why family education is so integral in the care of these children.”
For Mahan, who has authored a paper on factors predicting prenatal detection,14 family education begins before the baby is born.
“For me, it’s a conversation that often starts prenatally, because I often meet with these families prenatally or certainly start talking with them early on about the importance of longtime bracing, and I start that discussion at the first encounter,” Mahan said. “The serial casting and the initial correcting of the clubfoot, pretty much all families comply. They can almost see from the first cast the improvement of the foot. But once the foot’s corrected, the greatest challenge we have is to try and encourage the foot not to return to its clubfoot position, and the most reliable way to do that is consistency with the brace.”
Larry Hand is a writer in Massachusetts.
1. Smith PA, Kuo KN, Graf AN, et al. Long-term results of comprehensive clubfoot release versus the Ponseti method: which is better? Clin Orthop Relat Res 2014;472(4):1281-1290.
2. Brodsky JW. The adult sequelae of treated congenital clubfoot. Foot Ankle Clin N Am 2010;15(2):287-296.
3. Zhao D, Li H, Zhao L, et al. Results of clubfoot management using the Ponseti method: do the details matter? A systematic review. Clin Orthop Relat Res 2014;472(4):1329-1336.
4. Spiegel DA. CORR Insights: Results of clubfoot management using the Ponseti method: do the details matter? A systematic review. Clin Orthop Relat Res 2014;472(5):1617-1618.
5. Harmer L, Rhatigan J. Clubfoot care in low-income and middle-income countries: from clinical innovation to a public health program. World J Surg 2014;38(4):839-848.
6. Evans AM, Perveen R, Ford-Powell VA, Barker S. The Bangla clubfoot tool: a repeatability study. J Foot Ankle Res 2014;7:27.
7. Ford-Powell VA, Barker S, Khan MS, et al. The Bangladesh clubfoot project: the first 5000 feet. J Pediatr Orthop 2013;33(4):e40-e44.
8. Perveen R, Evans AM, Ford-Powell V, et al. The Bangladesh clubfoot project: Audit of 2-year outcomes of Ponseti treatment in 400 children. 2014 May 19. [Epub ahead of print]
9. Sutcliffe A, Vaea K, Poulivaati J, Evans AM. ‘Fast casts’: Evidence based and clinical considerations for rapid Ponseti method. Foot Ankle Online J 2013;6(9):2.
10. Harnett P, Freeman R, Harrison WJ, et al. An accelerated Ponseti versus the standard Ponseti method: a prospective randomized controlled trial. J Bone Joint Surg 2011;93(3):404-408.
11. Owen RM, Kembhavi G. A critical review of interventions for clubfoot in low and middle-income countries: effectiveness and contextual influences. J Pediatr Orthop B 2012;21(1):59-67.
12. Maripuri SN, Gallacher PD, Bridgens J, et al. Ponseti casting for clubfoot-above-or below-knee?: A prospective randomized clinical trial. Bone Joint J 2013;95-B(11):1570-1574.
13. Lykissas MG, Crawford AH, Eisman EA, Tamai J. Ponseti method compared with soft-tissue release for the management of club foot: a meta-analysis study. World J Orthop 2013;4(3):144-153.
14. Mahan ST, Yazdy MM, Kasser JR, et al. Prenatal screening for clubfoot: what factors predict prenatal detection? Prenat Diagn 2014;34(4):1-5.